Nurses, Midwives and Health Visitors
13.1 Nurses, midwives and health visitors play a vital part in the care of patients in hospitals, nursing homes and the community. They have constant and direct contact with patients, in most cases the service is provided throughout 24 hours, and they give more personal care than many other groups of staff. They are the largest staff group in the NHS and command the largest salary bill, accounting for over one-quarter of the total current expenditure in the NHS. For all these reasons the part that they play in the NHS is profoundly important.
13.2 In this chapter we discuss some of the main problems of nurses, midwives and health visitors put to us in evidence. We dealt with the allegation of increased numbers of administrators following the Salmon Committee Report in Chapter 4, and with community nursing in Chapter 7, and we touched on aides and manpower planning in Chapter 12. We concentrate here on roles, manpower requirements, an improved career structure for clinical work, and some aspects of education and research, but we start by commenting on the standards of care provided to patients. Much of what we say here applies equally to nurses, midwives and health visitors and our use of “nurse” and “nursing service” should be interpreted accordingly.
The Briggs Committee
13.3 In preparing this chapter we have been conscious of the major review of the nursing service undertaken by the Briggs Committee which reported in 1972. The Committee’s terms of reference were:
“to review the role of the nurse and the midwife in the hospital and the community and the education and training required for that role, so that the best use is made of available manpower to meet present needs and the needs of an integrated health service”.
The Committee made a detailed study of the role of the nurse and important proposals for the statutory framework of nurse education and training, manpower, conditions of work, reorganisation of nursing and midwifery functions, career structure, and research. We have drawn heavily on their work.
13.4 We are concerned that relatively little progress has been made on the major recommendations scheduled by the Committee for “immediate action” and not needing legislation, for example an effective manpower policy, increased recognition of clinical skills and a major drive to produce more nursing and midwifery teachers. Although some progress has been made, the “period of intense activity” envisaged by the Committee as occurring after their report did not take place. Indeed, it took seven years before legislation to set up the statutory framework recommended by the Briggs Committee was enacted.
Standards of care
13.5 We received much evidence expressing concern about declining standards of nursing care. It was often attributed to the structural changes arising from the Salmon and Mayston Committees’ recommendations and their alleged tendency to withdraw good clinical nurses into administration. We dealt with these points in Chapter 4. Further, in a submission to the Secretary of State for Social Services in October 1978 the RCN claimed that standards had been put at risk because of financial constraints, increased workloads and manpower shortages. They submitted that the main areas of risk were:
“in hospitals
untrained staff left in charge of wards inadequate supervision of learners neglect of basic nursing routines employment of agency staff
in the community
increased workloads which cause severe pressure on nursing staff with the consequent curtailment of time allocated to patients and learners abandonment of patient care programmes because of the need to cope with emergency cases and high dependency patients.”
13.6 These are serious matters. There is no doubt that nurses are under pressure in many places, and services to patients suffer. We refer later to increased workloads inherent in NHS policies and developments, training arrangements, and the balance of trained to untrained staff. Nurses expect to provide a high standard of care; their morale may be seriously affected if the standard of care they are able to offer their patients falls, and this may lead to some of them leaving the service.
13.7 In earlier chapters we have pointed out some of the difficulties in measuring quality in health care. Progress has been made by the profession in the evaluation of care through the use of nursing audit, research into clinical nursing methods, and staff appraisal schemes. Although some of these are in their infancy, the profession has shown it is well aware of the need for quality We were pleased to hear that the RCN has set up a working party to study standards of nursing care. We welcome this and other research initiatives and we hope that what we say in this chapter will contribute to improving both the quality of the nursing service provided to the patient and the nurse’s own role.
Role and numbers
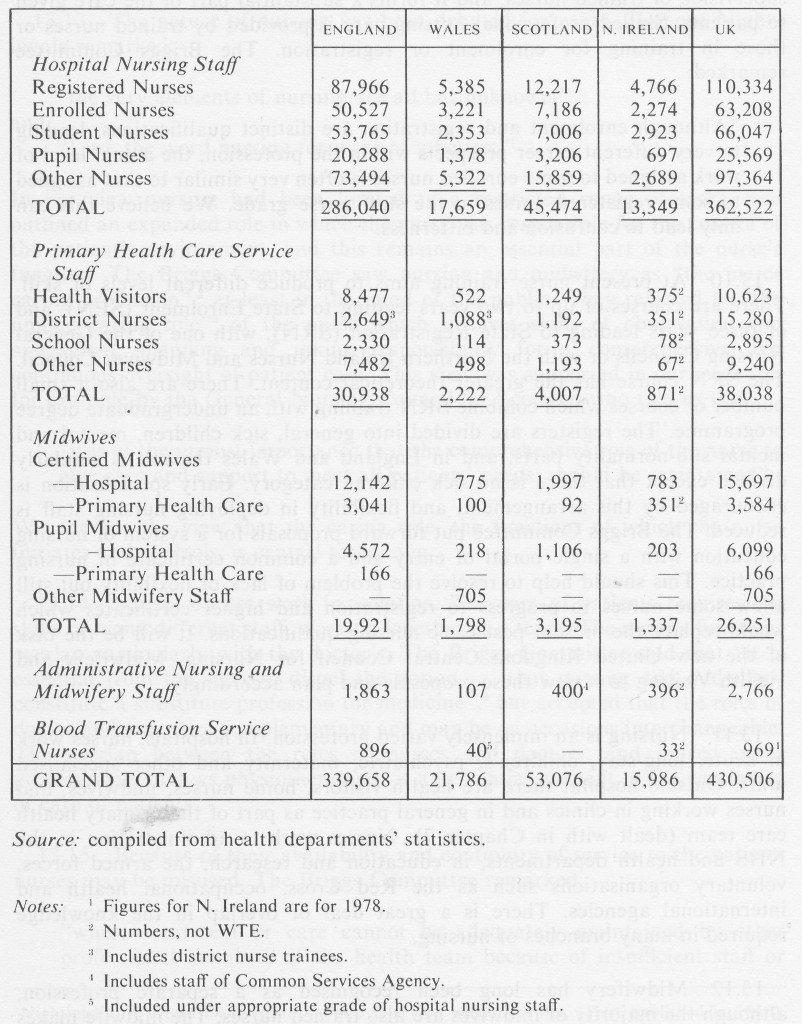
13.8 At present the NHS employs the equivalent of over 430,000 whole-time nurses, midwives and health visitors, approaching half of all NHS workers (see Table 13.1). The availability of nurses depends on such factors as the finance available for nursing budgets, the state of the local labour markets, recruitment and training policies and wastage. Demand for nursing care is related to morbidity and mortality trends, the organisation of care in institutions or community, and trends in medical treatment. These are constantly changing and the nurse’s role also changes. It has developed to take account of the increased nursing involvement in administration as well as changes in nursing practice. It overlaps with that of other health workers; for example, the nurse may carry out duties normally undertaken by a domestic worker, physiotherapist or doctor. All these factors make for difficulty in establishing the number of nurses the NHS needs.
TABLE 13.1 Numbers of Nurses: UK 1977
Whole-time equivalents
Role
13.9 Within nursing there are many levels of skill and different roles. Nursing in the NHS may involve providing unskilled but devoted care which might otherwise be given by relatives and friends. It is carried out by nursing assistants and auxiliaries with the minimum of in-service training, under the supervision of trained nurses, and it forms a substantial part of the care given to patients. Skilled professional nursing care is provided by trained nurses or those in training for enrolment or registration. The Briggs Committee remarked:
“Although enrolment and registration are distinct qualifications, leading to very different career prospects within the profession, the actual level of work assigned to some enrolled nurses is often very similar to that assigned to some registered nurses in the staff nurse grade. We believe this can only lead to confusion and bitterness.”
13.10 At present nurse training aims to produce different levels of skill. There are courses of up to two years leading to State Enrolment (SEN), and of three years leading to State Registration (SRN), with one of the General Nursing Councils or with the Northern Ireland Nurses and Midwives Council. The SRN course has the greater theoretical content. There are also a small number of courses which combine SRN training with an undergraduate degree The registers are divided into general, sick children, mental and mental sub-normality parts, and in England and Wales the roll is similarly divided except that there is no sick children category. Early specialisation is encouraged by this arrangement, and flexibility in deploying nursing staff is reduced. The Briggs Committee put forward proposals for a system of nursing education with a single portal of entry and a common certificate in nursing practice. This should help to resolve the problem of lack of flexibility but still allow some nurses to progress to registration and higher certificates which would replace the present post-basic nursing qualifications. It will be the task of the new United Kingdom Central Council for Nursing, Midwifery and Health Visiting to review these proposals and plan accordingly.
13.11 Nursing is an immensely varied profession. In hospitals, nurses work in acute, long-stay, children’s, psychiatric, maternity and other specialised Outside hospital there are health visitors, home nurses, midwives, and nurses working in clinics and in general practice as part of the primary health care team (dealt with in Chapter 7). Nurses work in administration in the NHS and health departments, in education and research, the armed forces, voluntary organisations such as the Red Cross, occupational health and international agencies. There is a great deal of overlap in the knowledge required in many branches of nursing.
13.12 Midwifery has long been recognised as a separate profession, although the majority of midwives are also trained nurses. The midwife makes her own judgments about the supervision, care and advice to women before and after childbirth. She is responsible for deliveries, and cares for the new-born and infants. It is part of her duty to detect abnormal conditions in mother and child, to decide when to summon the doctor, and to deal with emergencies in his absence. The Royal College of Midwives told us that in 75% of deliveries the midwife is the senior person present. Health education and counselling are an important part of her work. The role of the midwife may serve as a model of the extended role and clinical responsibility which nurses could carry.
13.13 The nature of nursing has been debated for years. Florence Nightingale remarked
“the very elements of nursing are all but unknown.” “I use the word nursing for want of a better.”
In her view nursing had been limited to a restricted range of tasks. She outlined an expanded role in which the nurse was responsible for the control of the patient’s environment, and this remains an essential part of the nurse’s function. The Briggs Committee saw nursing and midwifery as “the major caring profession”, at least in the mind of the public. They referred to “the unique caring role” of the nurse which involves skills of observation and assessment, planning and taking responsibility for a comprehensive and continuous oversight of patient care. This view was supported in our evidence, for example by the General Nursing Council for Scotland who told us that:
“it is of the utmost importance that the comprehensive role of the nurse to give care and support to meet all patients’ needs, should be maintained”.
We endorse the view that the caring role, the functions of which the nurse initiates and controls, is central to nursing.
13.14 Nurses do not work in isolation. The care of patients requires the skills of many different staff, working together as a team. The nurse’s functions overlap particularly with the doctor’s. The Briggs Committee said that “it is essential from the start to dispel the notion . . . that nursing and midwifery constitute a substitute profession for medicine”, but accepted that the roles of doctor and nurse are complementary and may be on occasions interchangeable. The overlap between the roles of nurses and doctors, and indeed other professionals such as physiotherapists, is an essential element in the continuity of care of patients.
13.15 Because of their availability and continuity of service to the patient, nurses may be misused. The Briggs Committee remarked:
“where treatment or care cannot be adequately maintained by other professional members of the health team because of insufficient staff or workload inadequate to justify the employment of specialist staff in small hospitals or units, nurses and midwives, on account of their availability and continuity of service, are usually the staff expected to attempt to take over the functions of other specialists”.
Nursing time may be eroded by nurses accepting other duties. The tasks of other groups should not as a matter of course be handed over to nurses simply because they are always there, and staff shortages whether of domestic or other professional staff should not be made an excuse for persistent misuse of nurses.
13.16 We were told of many different ways in which nursing roles are being extended and expanded. There is increasing recognition that the major health need of groups such as the chronic and long term sick, and the elderly, is for nursing care. The Regional Nursing Officers in England suggested to us that:
“Examination should be given to the possibility of extending the role of the nurse and enabling them to undertake tasks traditionally the province of the medical staff.. . . There is a need in some long stay care areas for nurses to take the lead. Nurses should be enabled and encouraged to prescribe nursing care programmes, including the mobilisation of other services such as physiotherapy and occupational therapy.”
This seems to us a logical extension of the nurse’s caring role. Adequate preparation for an extended role will be needed.
13.17 Extended roles for nurses are developing as a result of specialisation, for example in renal dialysis, care of spinal injuries, and special care baby units. Advances in medical science often require parallel advances in nursing care, and nurses working closely with doctors are pioneering new roles. During our visit to North America we found a growing interest in the role of the clinical nurse specialist. The health departments told us of similar appointments in the UK, usually at nursing officer or ward sister level. Specialist nurses may also have an advisory or an executive function in a health district. The RCN submitted a list of posts showing the range of specialties which have developed. While we recognise the danger that specialisation may lead to inflexibility, there is clearly a growing demand for specialist nursing skills in the care of certain groups of patients. We comment later on the need to reward special expertise, and on the preparation needed for advanced roles in nursing.
13.18 Nurses working in the community have long had a considerable degree of independence. For example, as we saw in Chapter 7, health visitors initiate their own visits, assess the development of children, undertake screening of the normal population, assess and care for the elderly, and advise on family It is possible that district nurses could undertake more first visits to patients in their home. An experiment carried out at the Woodside Health Centre in Glasgow suggested that decisions made independently by nurses and doctors about what to do for patients in the community were very similar.
13.19 In considering an extension of nursing roles in the community we were referred to the development of nurse practitioners in North America. We commissioned a study of the literature on nurse practitioners from Dr Jillian MacGuire. This showed that in North America a number of problems had stimulated the wider use of nurses in the community, including the shortage of doctors in general practice, maldistribution of health facilities, cost of health care, and pressure from the nursing profession itself. Nurse practitioners work mainly, but not exclusively, in primary care, and may be involved in hospital out-patient clinics. They work closely with doctors, but in some rural areas the nearest doctor can be many miles away and they have considerable independence. They take health histories from patients, act as first point of contact, provide teaching and counselling, and deal with a case load of patients with self-limiting diseases. Nurse practitioners have proved to be perfectly accept able to patients, and indeed are often felt to be more accessible than the doctor, particularly as in the main they operate in under-doctored areas. We do not see nurse practitioners as providing a second class medical service, but there is scope for further development in the roles of community nurses this side of the Atlantic.
13.20 In 1974 a joint working party of representatives of the nursing and medical professions and the DHSS identified a range of activities being undertaken by nurses both in the general and psychiatric fields which were clearly an extension of their normal functions. We consider that decisions about the respective responsibilities of the professions for different aspects of patient care should be made by the health departments after consulting the professions concerned, and with due regard to the interests of the patient and the level of knowledge and skill required. Where a function is identified as part of the nurse’s role it should be incorporated into basic or post-basic nursing education and be professionally supervised.
13.21 A main concern in our evidence was that any extension in the nurse’s role should not be at the expense of her caring functions. The GNC for Scotland warned us that “some technical procedures may distract from true patient care, and the nurse’s involvement in those which have this effect should not be encouraged”. The RCN told us that comments of community nurses in 1974 (which are still valid today) had shown that there was concern also in the community services at:
“the extended duties of both health visitors and home nurses, the running of immunisation and vaccination clinics, taking blood, performing vene-puncture, making ‘first assessment’ visits in place of the doctor and the using of new and more sophisticated equipment and drugs in patients’ homes where, in the case of an untoward event, there was no medical aid nearby”.
13.22 There are other risks in nurses taking on new tasks. The Briggs Committee pointed out:
“A nurse or midwife, whether working in the community or in a hospital, has a legal duty of care towards her patient. In giving this care she is required to exercise the degree of knowledge and skill which could reasonably be expected of one trained in her particular profession. If she falls below this standard and the patient is thereby harmed she will be regarded as negligent in common law and will be legally liable for the damage resulting from her negligence.”
Concern about their legal position may make nurses cautious about taking on new functions for which they have not been adequately trained. Extension of the nursing role needs to be planned and to take account of both training and staffing implications.
13.23 There will be able nurses who prefer to widen the scope of their work and make their careers in the clinical field rather than to move into administration or education. We believe that they should be encouraged to do so, and it seems to us to be a mistake to define or to confine the nursing role rigidly. Its development should be encouraged and experiment pursued, and we recommend that the profession and health departments take the necessary steps. It is clear that both the health departments and the professional organisations concerned are keeping a close watch on the position. They will need to ensure that new developments do not take place at the expense of the nurse’s caring role which is so important to patients and which itself is a prime candidate for expansion.
Numbers
13.24 Attempts have been made to calculate the numbers of nurses the NHS needs. Bed or population ratios, staffing norms, and workload indices based on patient dependency studies have been used, but none has proved wholly satisfactory. Minimum staffing standards have been set, for example in mental illness, mental handicap and geriatric nursing, but these do not purport to measure need. The Jay Committee found difficulty in making even a rough estimate of staffing needs for mental handicap. The DHSS commented to us that:
“Each health authority sets its own nursing establishments and to some extent engenders its own demand. Except for health visitors and home nurses where staff/population ratios have been recommended, the Department has not issued guidance to health authorities about assessing staffing needs.”
13.25 Recruitment of student and pupil nurses has fluctuated considerably in recent years. For example in England in 1976/77 there was an overall fall of 7.6% in numbers of nurses entering training, and in 1977/78 a further fall of over 21%. These fluctuations may reflect the financial difficulties of health authorities rather than an unwillingness of young people to enter nursing, and the 1978/79 figures showed a considerable improvement. Wide fluctuations of this kind make for difficulties in years to come and cannot be in the best interests of the service. There will be a decline in the number of 18 year olds in the population in the 1980s. Recruitment policy in the NHS will need to take account of this and the needs of mature students, male nurses and those from overseas. Also there should be better arrangements for training nurses who want to return to the service, for example after their children have grown up.
13.26 There are frequent complaints both in the press and in our evidence of shortages of nurses despite considerable increases in the numbers of nurses nationally over the years: between 1971 and 1977, for example, total numbers of nurses in England increased by about 23%. However, increases in numbers may be partly offset by a reduction in availability of staff: Table 13.2 shows that the increase between 1971 and 1977 fell to about 12% when this is taken into account. Further, the rate of increase has been tailing off: in 1976-1977 it was less than one-half per cent. Although the minimum staffing requirements for mental illness, mental handicap and geriatric nursing have been met (though these may need to be reviewed), and the number of health visitors has increased, the growth in district nursing is below the target set by the DHSS in 1976.
TABLE 13.2
Numbers of Nurses, Midwives and Health Visitors Adjusted for Availability: Hospital and Primary Health Care Services1:
England 1971-1977
| 1971 | 1972 | 1973 | 1974 | 1975 | 1976 | 1977 ! | |
| Total Staff (numbers) | 272,630 | 290,233 | 295,302 | 301,295 | 324,115 | 332,598 | 335,081 |
| Total Staff (adjusted2) | 272,630 | 276,412 | 280,050 | 276,752 | 297,843 | 305,505 | 306,300 |
| Total Staff (indexed3) | 100 | 106.5 | 108.3 | 110.5 | 118.9 | 122.0 | 122.9 |
| Total Staff (adjusted and indexed) | 100 | 101.4 | 102.7 | 101.5 | 109.2 | 112.1 | 112.4 |
| Changes in nurses’ conditions | 40 hour week | Revised leave | Additional | ||||
| 1st January 1972 | 1st April 1974 | Public Holiday |
Source: compiled from published and unpublished statistics provided by the DHSS.
Notes: ‘ Excluding tutorial staff, RHA headquarters staff, blood transfusion staff, nursing cadets and agency staff.
2 Adjusted figure = Total staff X (Annual Hours per WTE Staff Member for year) H- (Annual Hours per WTE Staff Member for 1971). •’ Index 1971 = 100.
13.27 Factors which have contributed to a reduction in nurses’ availability include a shorter working week, longer holidays, additional bank holidays and revised training schemes which have been widened to include community and psychiatric aspects. The benefits of a broader based training and ultimately greater flexibility are gained by some sacrifice of the service contribution during training. A sense of shortage of nurses may be produced by the greater throughput of patients in hospital, more people being cared for in the community, and nurses’ increasingly specialised and technical roles. Finally, the increase in the number of doctors which has taken place has resulted in greater demand for other services, including nursing.
13.28 Growth in total numbers may conceal local shortages, high wastage rates of learners, and difficulties in manning the relatively unpopular psychiatric and geriatric units. As with other NHS workers, the geographical distribution of nurses is uneven. Table 13.3 shows that in 1977 Scotland had over 68% more nurses and about 57% more midwives (though fewer health visitors) per 1,000 population than Oxford RHA. There are also variations within regions. A further factor is the number of overseas nurses particularly in the training grades. For example, in England in 1976 over 16% of all nurse learners were born overseas. The problems experienced by this group are similar to those of overseas doctors and some of what we say in Chapter 14 is relevant here.
13.29 The NHS has long been dependent on unqualified staff. About 50% of the nursing workforce is unqualified, fairly equally divided between nurse learners, nursing auxiliaries and assistants, some of whom receive only a short basic in-service training. The Briggs Committee welcomed “the increasing contribution” of these workers “in view of the differing levels of work to be done”. However, the high proportion of unqualified staff may produce problems; for example, the development of specialised units requires extra qualified staff and this may result in other units becoming more dependent upon auxiliaries and assistants. We were told of instances where unqualified staff were left in sole charge of wards, particularly in geriatric and psychiatric units, in which the patient/staff ratios were already low and demands on staff high. There has been little research into the effect of this on patient care, or into the best composition of the ward team in different settings for both service and educational purposes. We recommend that this should be rectified.
13.30 There is little or no nurse manpower planning to meet national requirements, though the mental and geriatric “leads” negotiated by the Whitley Council recognise the difficulties of recruitment in those areas. There are normally sufficient applicants for training and in practice the factors which most influence recruitment are probably the availability of funds and the local employment situation. The RCN pointed out:
“In spite of research the balance of the nursing team has been based on empirical considerations, the two most important being: which groups are easily available and how many can be paid for out of the current budget. In good times the service recruits, in bad it cuts back and replaces trained staff with untrained.”
The Briggs Committee considered that the absence of a manpower planning strategy was a serious deficiency, a view which we support.
TABLE 13.3 Nurses, Midwives and Health Visitors1 per 1,000 Population: UK 1977
Whole-time equivalents
| Nurses | Midwives | Health Visitors | |
| ENGLAND | 6.64 | 0.43 | 0.20 |
| Northern | 6.45 | 0.40 | 0.20 |
| Yorkshire | 6.67 | 0.40 | 0.19 |
| Trent | 5.90 | 0.38 | 0.19 |
| East Anglia | 5.90 | 0.43 | 0.17 |
| NW Thames | 6.82 | 0.43 | 0.22 |
| NE Thames | 6.93 | 0.49 | 0.17 |
| SE Thames | 7.33 | 0.46 | 0.21 |
| SW Thames | 6.98 | 0.34 | 0.23 |
| Wessex | 6.16 | 0.43 | 0.20 |
| Oxford | 5.50 | 0.40 | 0.25 |
| South Western | 6.82 | 0.42 | 0.19 |
| West Midlands | 6.10 | 0.43 | 0.19 |
| Mersey | 7.34 | 0.47 | 0.19 |
| North Western | 6.67 | 0.49 | 0.22 |
| WALES | 6.99 | 0.65 | 0.20 |
| SCOTLAND | 9.28 | 0.61 | 0.24 |
| N IRELAND2 | 9.00 | 0.87 | 0.27 |
Source: compiled from health departments’ statistics.
Notes: ‘ Excludes administrative staff, blood transfusion staff, agency staff and communitystudent nurses. 2 Figures for N. Ireland are 1978.
13.31 The major planning problem is to get the right number of nurses into the right places, particularly unpopular areas and specialities. The health departments are aware of this and have been working with the profession and the NHS to develop manpower planning expertise. Better methods of quantifying need might be a proper subject for study by the Health Services Research Institute we recommend in Chapter 17, but the most immediate requirement is that nurse managers at every level should have adequate manpower information on which to base their future plans. The development of computerised personnel records would be a great help here. We do not advocate the establishment of new and centralised planning machinery, still less that the health departments should control nursing establishments. We recommend that the health departments should undertake such central planning as is necessary, that is develop a national recruitment policy, assist the setting of standards and objectives, propagate good practice and ensure an adequate data base which will be of considerable importance to the new statutory educational bodies.
Clinical career structure
13.32 We recorded in Chapter 4 that the Salmon Committee’s recommendations on the senior nursing staff structure were often alleged to have resulted in a marked increase in the number of nurses employed on administrative duties. We concluded that the figures did not support this view. The structure was also unfairly blamed for the loss of experienced ward sisters, whereas it was demographic factors, such as changing patterns of marriage and child-bearing and the changed expectations of women in society, which were the main influences on the availability of ward sisters and the length of their working lives.
13.33 A workforce as large as nursing’s must be efficiently managed and this requires the involvement of many nurses in planning and decision making processes. A nurse should continue to be a member of management teams at all levels, and we agree with the RCN that the “concept of the team of equals must not be lost”. Nurse administrators will often need supporting staff to do their jobs properly, and we hope that health authorities will bear this in mind when considering their needs for clerical staff.
13.34 A major concern in the evidence from both medical and nursing organisations was that career prospects for nurses in clinical work should be improved. The British Association of Oral Surgeons, commenting on the Salmon structure, said that:
“This system, which requires experienced ward sisters to abandon clinical nursing and enter the administrative field in order to obtain promotion, aggravates the serious skilled nursing shortage … a career structure which offers high levels of promotion in clinical nursing should be reintroduced.”
We have referred to the way in which clinical nursing roles are developing, and the support for this of the regional nursing officers in England. The RCN told us that:
“there is a need to identify new roles for nurses as specialists and consultants, in different spheres of practice . . . This proposed extension of the role of the nurse is seen primarily as a means of promoting high standards of care; it would also provide an avenue of advancement for nurses who wish to continue in clinical work. The RCN believes that this development should proceed in two stages. The role of the nurse specialist is already capable of identification . . . The role of the nurse consultant should be the subject of research”.
At present the nurse who wishes to continue with and specialise in clinical work will suffer financially, as can be seen from Table 13.4. We discuss below ways in which career prospects in clinical nursing could be improved.
13.35 A satisfactory career structure in clinical nursing should be linked to the establishment of criteria for the evaluation of clinical expertise by a systematic analysis of clinical nursing functions. It seems to us that rewards in clinical nursing should depend more on a developing expertise and growing responsibility for clinical decision making than on a line responsibility for the management of other workers. In the process of developing satisfactory clinical career prospects, existing relativities may need to be disturbed.
Relationship Between Main Groups: England 1978
Administration Education Clinical2
Regional Nursing Officer (£10,866)
Area Nursing Officer (£10,266)
District Nursing Officer (£9,930)
Regional Nurse (£8,430)
Area Nurse(£8,073) Director of Nursing Education (£7,656)
Divisional Nursing Officer (£7,209)
Principal Nursing Officer (£6,516)
Senior Tutor (£5,403)
Senior Nursing Officer (£5,277)
Tutor (£5,028)
Nursing Officer2 (£4,848)
Clinical Teacher (£4,695) Nursing Sister/Charge Nurse (£4,695)
Staff Nurse (£3255)
Source: compiled from published and unpublished statistics provided by the DHSS.
Notes: ‘ Maximum salary for the highest grade in each category at April 1978.
2 There are a comparatively small number of clinical nurse specialists who are, in the main, graded as nursing officers.
13.36 A clinical career structure must be based on the staff nurse and ward sister grades and it is essential that their roles are reviewed and modified in the light of advances in nursing care. The importance of the team approach to nursing care giving co-ordinated physical and psychological care was stressed by the Briggs Committee, and we referred above to the need for research into the composition of the ward team. We welcome the research which is being undertaken into methods of organising patient centred nursing care and the roles of the ward sister and nursing officer.
13.37 There seem to be the following approaches to improving career prospects for nurses specialising in clinical work:
- revision of the ward sister’s salary scale to provide incentives for distinction or excellence in clinical practice;
- development of the existing nursing officer role to approach more closely the model originally envisaged;
- developing specialist and expanded roles for nurses on the lines referred to in paragraphs 13.16-13.23;
- linking teaching and research with clinical work.
The first approach is a matter for the Whitley Council, but the comparatively unfavourable position of nurses employed on clinical work is clear. One possibility would be the introduction of an open system of distinction awards on the lines of the one that applies to hospital consultants. This would involve developing criteria for clinical excellence which could include factors such as innovation in clinical methods, research and teaching.
13.38 The Salmon Committee envisaged that the nursing officer in the hospital would be in charge of a unit, and would be responsible “for seeing that patient care is of a high order, that the requirements for nurse education are met and that the unit is efficiently managed.” Her functions would include keeping abreast of clinical developments, advising unit nursing staff on nursing practice and helping to solve problems of patient care, as well as dealing with managerial matters such as deployment of staff and arrangements for nurse education.
13.39 It seems to us that the nursing officer should have a satisfying role with combined professional, administrative and personnel functions. However, her professional functions of acting as consultant in nursing practice, developing new ideas and methods, and teaching have emerged only in a few places. There are a number of reasons for this. First, the management content of the role is often so demanding that little time is left for clinical involvement, and training for nursing officers has often emphasised the management role to the exclusion of preparation for an advanced clinical role. Second, the medical profession have traditionally consulted the ward sister, and the Regional Nursing Officers told us that “the Nursing Officer has in most cases been ‘relegated’ by medical staff to administrative duties only”. Third, there is a real difficulty for grades above ward sister acting as consultants and advisers on clinical care if they do not take responsibility for the care of individual Expertise and special knowledge are quickly outdated. In the present system the ward sister has effective control of the clinical nursing care of patients in her ward, while the nursing officer has limited access to patients and her role as consultant has no base. She rarely has training in research methods and the clinical teacher may effectively exclude her from a teaching role.
13.40 We consider that the original concept of the nursing officer has much to commend it and we recommend that her clinical role should be developed along the lines envisaged by the Salmon Committee. There is scope for experiment, for example in the nursing officer specialising in either the clinical or the management aspect of her role. It seems to us that a clinical nursing officer should assume responsibility for a group of selected patients and combine clinical, research and teaching functions.
13.41 We have already referred to the development of nurse specialist/consultant posts in the hospital service. There was some criticism of this development in our evidence. As COHSE said:
“Who is going to consult the nurse consultant? We don’t think that the ward sister will. It would undermine the role of the sister. In fact it would change her role beyond recognition – the key role in the nursing structure. Perhaps the doctor will consult the nurse consultant then? We don’t think so. The doctor will also want to consult the ward sister – and rightly so when he or she wants information about the patient.”
While we think this overstates the case, healthy scepticism about the creation of new jobs is certainly desirable. On the other hand nurses may well acquire considerable expertise in a special area, for example in the control of infection, which can and should be put to good use elsewhere in the service. The nature of this role and the specialist’s relationship with her colleagues will need to be worked out. This is a matter for the profession itself and research will assist it in dealing with these issues. The grading of nurses who develop specialist or consultant roles is of course for the Whitley Councils to determine, but we would expect that nursing officer or above would often be appropriate.
13.42 Hard and fast rules will prevent the best use being made of highly skilled manpower. The 30 years of the NHS have seen the emergence of many professional groups in response to service need, and there is no reason why this should not occur in nursing also. The nurse is to some extent in the same position as the newly qualified doctor: she has had her general training but her usefulness will be further improved by experience and the development of specialist knowledge and skills. We recommend that the development of such specialisation, both in the community and hospital, should be encouraged. The continued expansion and improvement of post-basic education will be essential and we refer to this later.
13.43 The fourth approach to improving the career prospects of nurses engaged in clinical work is to combine clinical work with teaching and We see this combination at different levels in both the ward sister’s and clinical nursing officer’s roles, and we suggest that joint appointments between the schools of nursing and the nursing service could be developed with
benefit to both nursing education and patient care. We deal with education and research in the next section.
13.44 The approaches to improving the nurse clinical career structure considered above are not exclusive. They complement each other and all four should be encouraged. This should do much to ensure that the nurse who wants to remain in the clinical field will have a worthwhile and rewarding job.
Education and Research
13.45 The Nurses, Midwives and Health Vistors Act 1979 is a notable, if long-awaited, contribution to nursing education. It provides for a single United Kingdom Central Council supported by powerful national boards in each of the four parts of the UK which replace the existing separate bodies responsible for the education and regulation of the professions. The Central Council has a duty to prepare and maintain a central register of qualified nurses, midwives and health visitors, and to determine the education, training and other requirements for admission to the register. Such a structure is consistent with the Briggs Committee view that:
“what the branches of a united profession have to give to each other is more significant and more fundamental than the respects in which they differ. We believe that a structure can be created in which essential differences are safeguarded within the overall unity”.
We endorse this view and welcome the Act.
13.46 The Briggs Committee proposed a broad training for all entrants leading to a certificate of nursing practice fitting “a nurse to work in any field at the basic level of membership in a nursing team”. Experience in different fields of nursing during training would help to break down the barriers that exist at present, provide a greater flexibility in deployment, and promote a better understanding of the diverse professional roles in an integrated service. The Committee went on to recommend courses at registration and higher certificate level for more specialised roles. It will be part of the task of the new Central Council to review these recommendations in the light of more recent educational and professional developments. Reports from the Court, Jay and Warnock Committees have implications for paediatric and mental handicap nursing and midwifery and health visiting. In addition the EEC requirements will affect the range of experience required.
Nurse learners
13.47 Student and pupil nurses are employees of the NHS and form some 25% of the total nursing staff employed in the hospital service. Not surprisingly there are occasions when patient and educational needs conflict. Training arrangements should be designed to minimise pressures on students and pupils, and provide adequate support and supervision by qualified staff. There has long been an argument about whether nurse learners should be bona fide students rather than employees, and it appeared also in our evidence. The General Nursing Council (GNC) for England and Wales told us that their concern for the nurse learner could be expressed in two related questions:
“(A) is the trainee nurse being recruited/employed for her immediate availability as a worker in hospital or for her future potential as a trained nurse?
(B) is the trainee nurse being trained/educated for her own benefit or for the overall needs of the NHS?”
The truth is that the nurse learner is being recruited for both her availability as a worker and her future potential as a qualified nurse; and for both her own benefit and the overall needs of the health service. However, there is inherent conflict in these aims.
13.48 The GNC for England and Wales drew to our attention the proportion of time which learners can contribute to service needs after educational requirements have been met and the problems this creates for nurse managers, teachers, ward sisters and the learners themselves. The GNC recommended that the trainee should remain an employee. The RCN did not agree:
“recent legislation, relating to the employment situation has made untenable the student/employee status of the nurse learner … In urging that nurse learners should be accorded student status the RCN is not departing from its strongly held view that nursing can only be taught and learnt in the context of giving care. In the course of training students will contribute to the service; this does not require that they be employees of the service authority . . . There is need to review the status of nurse learners as a matter of urgency”.
13.49 A Working Group was set up by the DHSS following the Briggs Committee report to consider the status of the nurse learner and it supported the view of the Committee that:
“students should not consider themselves as nor be considered as part of the ordinary labour force of the National Health Service”.
The Working Group concluded that although there should be no immediate change in the present “employee” status, the question should be pursued by the new educational bodies. We support this conclusion. We consider it essential to the quality of the service that patients should not be nursed by untrained staff unless they are adequately supervised, and that the nurse’s basic education should prepare her for an exacting future role. We also set out some broad principles:
- clinical practice is the “core” of nursing education;
- clinical practice is best taught by practising nurses in real situations;
- in learning practical skills the nurse learner will inevitably give service to the NHS whatever her status;
- adequate demonstration of skills and supervision of practice must be given by trained staff and standards of supervision need to be established;
- whatever the nurse learner’s status her educational needs must be safeguarded.
Post-basic training
13.50 Nursing, midwifery and health visiting have a long and honourable history of post-basic preparation for advanced roles in the profession. These include preparation for management, nurse teaching and clinical roles in hospital and the community. At present a number of different bodies have responsibility and courses are organised in higher and further education establishments, within the NHS and by the Royal Colleges. The United Kingdom Central Council for Nursing, Midwifery and Health Visiting will be able to take a broad view of both basic and post-basic education and a great deal of rationalisation should be possible.
13.51 Basic nursing education can only be a foundation. It needs to be followed by systematic updating and more advanced preparation for specialised roles through post-basic educational programmes. We approve the diversity of provision that is available. In particular we welcome the work of the Council for the Education and Training of Health Visitors since its inauguration, the introduction of mandatory training for district nurses by the Panel of Assessors for District Nursing, and the progress made by the Joint Board of Clinical Nursing Studies (JBCNS) since it was established in 1972. By the end of 1978 the JBCNS had approved 375 education centres, and outline curricula had been prepared for 64 courses leading to a certificate and a further 16 leading to a statement of attendance. Although this represents considerable progress there is room for further development.
13.52 We were told that financial support for post-basic nursing education was not always available. We believe that nurses, midwives and health visitors should be adequately prepared for advanced roles in clinical specialties, education, management and research. Post-basic education is essential, and we recommend that health authorities should establish budgets and develop programmes for their nurses.
Nurse teachers
13.53 We referred earlier to the Briggs Committee recommendation that pending the establishment of the new educational bodies:
“As a matter of utmost urgency, a major programme to increase the nurse and midwife teaching strength should be launched.”
This has not happened. The number of qualified teachers has been slow to expand despite their relatively favourable position compared with the financial clinical grades (see Table 13.4). The DHSS told us that although attempts have been made to increase the numbers, a high wastage rate has kept the ratio of qualified teachers to learners constant at about 1 to 25 since 1972. While the ratio has improved in Scotland from 1 to 36 in 1972 to 1 to 21 in 1977, it still falls substantially short of the 1 to 15 aimed at for Scotland. The ratio in Northern Ireland was 1 to 17 in 1977, and in Wales 1 to 23 in 1978.
13.54 The delay in implementing this specific recommendation of the Briggs Committee may in part have caused the uncertainty about the future which has affected the supply of nurse teachers. The GNC for England and Wales highlighted three problems; inadequate support for the development of new curricula, shortages of trained staff in clinical practice, and shortages of qualified teachers carrying clinical responsibilities. The GNC recommended a number of measures to solve these problems, but they are still under discussion with the DHSS. This lack of progress underlines our concern at the apparent failure of the parties involved to recognise the need for urgent action in developing nursing education and increasing the number of nurse teachers.
13.55 Part of the difficulty in recruiting sufficient nurse teachers has undoubtedly been that once a nurse goes into education she may effectively lose touch with clinical work. One solution to this problem would be to ensure that tutorial staff also carry a clinical load in the same way as university medical teaching staff have clinical responsibilities for NHS patients. It seems to us that joint appointments between service and education have several advantages: they enable the teacher to keep in touch with clinical work and to avoid a too theoretical “classroom” approach to teaching; the nurse who is interested in teaching but does not want to give up her clinical work need not do so; and the more attractive salary scales at present available to the tutorial grades might be open to the nurse interested in clinical work who wished to improve her career prospects. We have not gone into this in depth, but although apprehensions have been expressed about such appointments we recommend that developments in joint appointments between schools of nursing and the service should be vigorously pursued. We envisage that this role could combine clinical research and teaching, and it could be seen as an expansion of the clinical teacher’s role or as specialisation within the nursing officer role. In addition we consider it important that full-time clinical nurses should receive adequate training for their teaching role, and should be encouraged, say by honorary appointments or attachments to nursing schools, to pursue it. The increase in nurse teachers recommended by the Briggs Committee seven years ago, a recommendation which we endorse, is now urgent, and unless it takes place the other reforms of nurse education proposed by the Committee will not be possible.
Nursing research
13.56 Although nurses are the largest staff group in the NHS, few nursing methods have been examined for their effectiveness. A much more critical approach towards nursing is required, and nurses themselves should obviously be involved in researching it. We were pleased to learn of recent improved arrangements for enabling nurses to undertake research. In particular the RCN Research Society are encouraging research-minded nurses. There is a useful dissemination of research findings in the RCN research series, and in the Index of Nursing Research and Nursing Research Abstracts published by the DHSS. The Nursing Research Unit at the University of Edinburgh has an outstanding reputation and there is a growing amount of research associated with departments of nursing in the universities and polytechnics. We welcome the establishment of the Nursing Education Research Unit at Chelsea College, the Nursing Practice Research Unit at Northwick Park Hospital, and the World Health Organisation collaborative units for research on the nursing process at Edinburgh and Manchester Universities. There is heartening evidence in the literature and in practice that nurses are beginning to apply research findings in their work, in for example, the prevention of pressure sores, feeding the unconscious patient, the management of pain, and promotion of continence.
13.57 Despite this it seems to us that there is considerable scope for developing nursing research further. However, competent researchers cannot be created overnight. Nursing fellowships are available from the health departments and though numbers awarded have risen slightly, demand from well-qualified applicants has been small. We hope that the education arrangements recommended by the Briggs Committee will, in due course, provide a basis which will enable nurses with an interest in research to develop their potential. We should also like to see health authorities do more to encourage their nurses to assist in, or undertake themselves, perhaps on a part-time basis, approved research projects. This is, after all, the way that much of the clinical research undertaken by doctors is arranged. We consider that our earlier suggestion of incorporating a research function into clinical and teaching roles will assist development in this field. We say more about research in Chapter 17.
Conclusions and Recommendations
13.58 It is difficult to overestimate the importance of nursing services in the NHS. Nurses are the most numerous and the most costly group of health workers, but more important is the close relationship they have with patients. We were therefore disturbed by criticisms of standards of care made by the Royal College of Nursing and referred to in our evidence.
13.59 Our whole approach to the questions discussed in this chapter has been coloured by the report of the Briggs Committee. The Committee dealt with matters which we would otherwise have had to discuss. We were disappointed that more progress had not been made with implementing their recommendations. There was disagreement in the profession over some aspects of the Committee’s recommendations, and, like many other desirable reforms, the follow-up work on the report was held up by NHS reorganisation. In particular little progress has been made on the clear recommendation, which we endorse, for more nurse teachers. However, the Nurses, Midwives and Health Visitors Act 1979, which sets up the new statutory educational bodies is a welcome, if long-awaited, development.
13.60 The profession is going through a difficult period. It has suffered major structural changes following the Salmon and Mayston Reports and was considerably influenced by the management changes introduced at reorganisa Nurse administrators fulfil a necessary function, but to do their jobs properly need adequate supporting staff. The role of the nurse is varied and it is being further extended and expanded by, for example, research into the caring function of the nurse, and development of specialisation. There is a need to improve the clinical career structure, and to encourage flexibility in the way nurses work.
13.61 Developments in nurse education have been delayed pending the new statutory bodies. The Central Council for Nursing, Midwifery and Health Visiting will need to review both basic and post-basic education. Linked to this we see a need to develop the research capacity of the profession.
13.62 We recommend that:
- the profession and the health departments should encourage and pursue experiments in the development of the nursing role (paragraph 13.23);
- research is required into the effect of the use of unqualified staff on patient care and into the best composition of the ward team in different settings (paragraph 13.29);
- the health departments should undertake such central manpower planning as is necessary, that is develop a national recruitment policy, assist the setting of standards and objectives, propagate good practice and ensure an adequate data base which will be of considerable importance to the new statutory educational bodies (paragraph 13.31);
- the clinical role of the nursing officer should be developed along the lines envisaged by the Salmon Committee (paragraph 13.40);
- the development of specialist knowledge and skills, both in the community and hospital should be encouraged (paragraph 13.42
- health authorities should establish budgets and develop programmes of post-basic nursing education for their staff (paragraph 13.52);
- developments of joint appointments between schools of nursing and the service should be vigorously pursued (paragraph 13.55).