Can the NHS handle the outsourcing of clinical services?
Executive Summary
- The NHS now contracts out the provision of health services to the private sector to the tune of over £20 billion a year, or a fifth of the total healthcare budget. Although a significant proportion of this is made up of contracts with Dentists, Pharmacies, Opticians and General Practitioners, the newest and biggest area of outsourcing is in relation to those services which the NHS, until very recently, used to provide directly: community health services and secondary care.
- Over the last four years there has been a 50% increase in the amount spent in the private sector on these services by local commissioning bodies and NHS trusts, from £6.6bn in 2009 to £10bn in 2014.
- This trend looks set to continue with the introduction of the Health and Social Care Act 2012 which places a requirement on Clinical Commissioning Groups (CCGs) to put services out to competitive tender.
- Administering, monitoring and enforcing these contracts is costly. We estimate that there are now some 53,000 contracts between the NHS and the private sector, including contracts for primary care services. These contracts, as well as the contracts with NHS providers, are arranged and administered by 25,000 staff working in CCGs, Commissioning Support Units (CSUs) and NHS England’s local area teams, at an annual cost of £1.5bn.
- The safety and quality of healthcare in England now depends increasingly on how effectively the NHS monitors and enforces this myriad of contracts with the private sector. But contracting for healthcare is highly problematic. Asymmetry of information makes it almost impossible for a commissioner of services to know whether a provider is delivering according to the terms of the contract, or is cutting corners or reducing quality in order to gain extra revenue.
- There have been a number of documented high-profile cases, such as Winterbourne View and Serco’s out-of-hours primary care contract in Cornwall, where the NHS has failed to manage contracts with private sector providers effectively. The Public Accounts Committee has identified significant weaknesses in central government’s general capacity to monitor and enforce contracts with large private companies and Monitor, the economic regulator of the healthcare market, has identified similar serious weaknesses in the capacity of local CCGs.
- However, little is known about how CCGs inspect and enforce contracts with the private sector. Using available official data, and data from 181CCGs which responded to a survey, we identified the following:
- Out of the total of some 53,000 contracts which the NHS holds with private providers of care, the 211 CCGs currently hold over 15,000. Expenditure by CCGs on contracts with the private sector amounted to £9.3bn in 2013-14, 16% of their £65bn budget.
- Given the complexity of monitoring contracts for healthcare, regular site visits to private providers of NHS services ought to take place. However, there is little record of the number of site inspections which CCGs carry out in relation to the contracts that they hold. Out of those which responded to our survey 109 (60%) did not record how many site inspections they undertook, or were unable to say how many they had done. Of even greater concern, 22 (12%) did not carry out any site inspections.
- CCGs remain the contracting bodies, with statutory responsibilities, but most of them have contracted out their contract monitoring function to Commissioning Support Units or CSUs. CSUs, which between them employ some 8,500 staff, are at present technically part of NHS England, although the government intends them to become private companies by April 2016. Most CCGs also share contracts with other CCGs.
- These complex arrangements are the reason why many CCGs said they were unable to answer questions about the number of contracts they hold or how many site visits have been undertaken.
- In a 2013 study of CCGs Monitor found that they were reluctant to enforce the terms of contracts for fear of exacerbating the financial situation of providers. Our survey supports this finding. We found that only seven out of the 15,000 contracts had been terminated because of poor performance and only 134 contract query notices had been issued. Only 16 CCGs had imposed any form of financial sanction on private providers.
- The picture which emerges from these facts is of an NHS poorly equipped to ensure that healthcare services outsourced to for-profit providers will provide safe, high-quality care and good value for money. At the same time accountability for the handling of the £9.3bn which CCGs are now spending annually on non-NHS providers of NHS care is being thwarted by the outsourcing of the contract monitoring work for which CCGs are legally responsible to unaccountable Commissioning Support Units which are soon to be privatised.
Recommendations
If the outsourcing of NHS clinical services to the private sector is to continue, and if patients and the public are to be confident that standards are being met and that value for money is achieved, a number of measures need to be taken to address the issues raised in this report.
- NHS England should commission an independent audit of CCGs’ capacity to monitor and manage contracts with non-NHS providers before any further major contracts are arranged.
- NHS England should reconsider its plans to privatise the contract monitoring of NHS contracts. CCGs are the statutory bodies responsible for enforcing contracts between the NHS and the private sector, not CSUs, which remain unaccountable if anything goes wrong. This problem will be exacerbated if CSUs become private companies, as is intended, from April 2016. With nearly £10bn worth of contracts with the private sector already in place, it is vital that statutory bodies are genuinely responsible and accountable for ensuring that private providers deliver according to the terms of their contracts.
- To improve transparency CCGs should be required to publish regular performance data on the number and value of contracts they hold, how they know whether contracts are performing well, the number and type of staff they employ to monitor and enforce contracts, and the amount of any over-payments they may have made to providers due to error or fraud.
The contracting NHS: key facts
- 53,000 estimated number of contracts held between the NHS and the private sector for healthcare in England, including for primary care services.
- £22.6bn total value of NHS contracts with the private sector, including primary care services.
- 24% percentage of NHS England’s total budget of £95bn which is spent in the private sector, including for primary care services.
- £9.3bn amount spent by CCGs on contracts with the private sector for NHS services in 2013-4.
- 16% percentage of the total Clinical Commissioning Group budget of £65bn which is now spent on the private sector.
- 15,000 estimated number of contracts between CCGs and the private sector.
- 90 average number of contracts with the private sector held by each CCG.
- 25,000 number of staff employed in CCGs, CSUs, and NHS Local Area Teams to commission, administer and enforce NHS contracts.
- £1.3bn combined budget of CCGs and NHS England Local Area Teams for commissioning, administering and enforcing NHS contracts.
- £700m amount spent by CCGS on CSUs to administer, monitor and enforce their contracts with NHS and private sector providers.
The contracting landscape
- Until 1990 the NHS was a complex but unified organisation, comparable to a very large multinational company. Its services were planned and funded centrally; service delivery was organised through a system of regional and district branches of the central NHS management. Good performance was achieved through line management but relied implicitly on trust, which in turn rested on a service ethos grounded in a shared commitment to prioritising the wellbeing of patients.
- In 1990 the NHS and Community Care Act introduced the purchaser-provider split and an ‘internal market’ in which NHS acute hospitals, mental health and ambulance services became semi-independent ‘trusts’, operating under non-enforceable contracts with local ‘purchasers’. (Many NHS hospital trusts send patients for treatment in local private hospitals to avoid financial penalties for not treating them within 18 weeks of referral, as occurred in 2014 when Musgrove Park Hospital in Taunton sent patients for cataract surgery to the private operator Vanguard ) In addition, between 2004 and 2006 new contractual arrangements were introduced between the NHS and private providers of primary care services, dentistry, pharmacy, general practice and ophthalmic services.
- By 2013, when the Health and Social Care Act came into effect, the market had ceased to be purely internal; private providers were now able to compete to provide NHS clinical services, using legally enforceable contracts. Clinical Commissioning Groups (CCGs), which now took on the PCTs’ purchasing function, were required to put contracts out for competitive tender to the private sector.
- The Department of Health has acknowledged that it does not keep a central record of the total number of contracts which underpin this new NHS market.2 Looking at various data sources, including a Freedom of Information (FOI) survey we conducted of all 211CCGs, we estimate that there are now some 53,000 contracts between the NHS in England and private sector providers. This includes the contracts which are held by NHS England with dental practices, pharmacies, ophthalmic service providers and general practices, all of which are independent businesses, as well as the contracts with non-NHS providers held byCCGs.
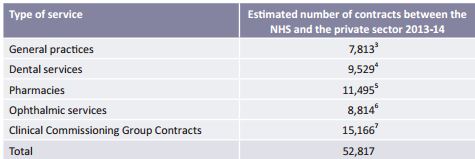
Table 1 The number of contracts between the NHS and the private sector for the provision of healthcare services - Hospitals and other providers may themselves also commission services; e.g. hospitals may have contracts with private laboratories to provide diagnostic services, or with other hospitals (including private hospitals) for the treatment of some of their patients, in effect subcontracting some of the work they are themselves under contract with CCGs to provide. However, we have been able to find no information on the number of these contracts.
- According to the Department of Health’s accounts for 2013-2014 the total expenditure on contracts for health care with the private sector amounts to £22bn, or almost a quarter of the £95bn allocated to NHS England to provide health care. The value ofCCG contracts with the private sector now amounts to £9.3 billion, or around 16% of the £65 billion allocated toCCGs. Unlike primary care services (dentistry, pharmacy, ophthalmic services, and general practice),CCG contracts with the private sector are for services – community health services and secondary care – which, until recently, the NHS provided directly.
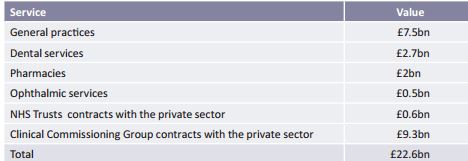
Table 2 Expenditure on contracts with the private sector for the provision of NHS care in 2013-14 - As Figure 1 demonstrates,
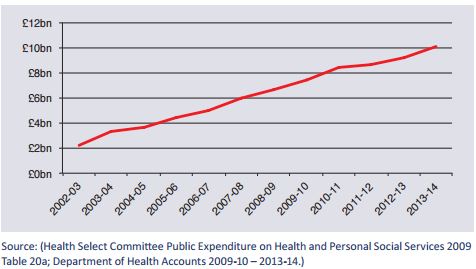
Growth in the expenditure of PCTs/CCGs and NHS Trusts
on private sector provision 2002 – 20141since the opening up of NHS services to the private sector, following the Blair and Brown government reforms, there has been a rapid increase in the number and value of services outsourced by local commissioning organisations to the private sector. For example in the last five years there was a 50% increase in the amount spent by PCTs/CCGs and NHS trusts on non-NHS providers, increasing the total spend from £6.6bn to £10bn. We expect that this trajectory will continue under the provisions of the Health and Social Care Act 2012.
- The nature of the companies with which the NHS contracts is relevant when considering the capacity of CCGs and the NHS to monitor the contracts, as it can affect the nature of the contractual relationship. Any private company must make a profit in order to survive, and the Companies Act requires company staff to prioritise the interest of shareholders. These incentives and pressures can impact on how the provider behaves: if profits can be increased (or losses reduced) by cutting the quality of services to patients, or by cutting corners, there is an incentive to do it, and this may be enhanced by pressure from managers who have corporate profit targets to meet.
- CCGs also hold contracts with NHS Trusts and other NHS bodies, but due to the fact that they have different governance and accountability arrangements and have inherited a public service ethos these contracts can often still be successfully managed through relational or trust-based contracting arrangements.
- The ownership structure of firms is also relevant. Competitive markets are inherently dynamic and firms of any kind, from large multinationals to small family businesses, may have problems which impact on patients. Firms owned by private equity (i.e. companies whose shares are not publicly traded), however, are a distinctive category because private equity companies rarely intend to retain ownership of other firms in the long term: they typically seek to realise a medium-term return on the other companies they own through high returns on debt or through restructuring and resale. The problems to which this can sometimes give rise were exemplified by Castlebeck Holdings, which was dismantled after the scandal at Winterbourne View:
Castlebeck Care (Winterbourne View)
Winterbourne View was a private hospital near Bristol for adult NHS patients with mental disabilities, built and operated by Castlebeck Care. In May 2011 a BBC reporter secretly filmed patients being grossly abused by the staff. The subsequent Serious Case Review reported that ‘the majority of staff at the hospital were unregulated support workers who are not subject to any code of conduct or minimum training standard. Over time Winterbourne View Hospital became a Support Worker-led hospital…’.
Contract monitoring had been virtually non-existent, and regulation had not compensated for its failure. The Care Quality Commission (CQC) had ignored three warnings from whistleblowers and had carried out three inspections in the previous year which failed to find any evidence of abuse.
A subsequent CQC inspection of 23 of Castlebeck’s other hospitals and homes identified several ‘company-wide themes’ including ‘lack of training for staff’; ‘inadequate staffing levels’; ‘poor care planning’; and ‘failure to notify relevant authorities of safeguarding incidents’. The Serious Case Review found that ‘even though the hospital was not meeting its contractual requirements in terms of the levels of supervision provided to individual patients, [the NHS] commissioners continued to place people there’.
Behind these failures lay the fact that with an annual turnover of £55m Castlebeck was carrying £428m of debt on which it was paying interest of £38m a year, resulting in a trading loss of £19m in 2008 and £10m in 2009. This financial model reflected the purchase of Castlebeck in 2006 by a private equity company registered in Jersey. The surplus was going to the owners of the debt, leaving management struggling to cut costs.
- The nature of the businesses which contract with the NHS to provide healthcare services varies considerably. In the dental sector, the NHS mainly holds contracts with small or medium sized businesses, whilst NHS pharmacy contracts tend to be held with larger multiple chains such as Boots or Lloyds. This is also the case with NHS ophthalmic services, where chains such as Boots, Vision Express and Specsavers dominate. On the other hand the contracts with General Practices are mainly with small independent providers which also receive financial support from the NHS in relation to their premises and IT infrastructure; only a very small proportion currently belong to corporate chains.
- No comparable information is publicly available about the non-NHS providers of services toCCGs. In order to establish the nature of these we looked at those licensed by Monitor under the Health and Social Care Act to provide NHS Clinical Services toCCGs. In 2014 59% of these companies were for-profit providers and out of these 58% were backed by private equity.
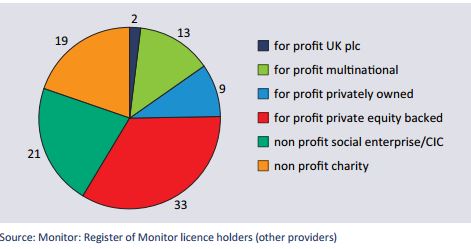
Figure 2 Provider companies licensed by Monitor in October
2014, by company type (n=97) - In relation to each of the NHS’s 53,000 contracts, resources are needed in order to monitor and enforce them, otherwise there is no guarantee that the provider of the contract will deliver safe and effective care. The Health and Social Care Act placed the commissioning of NHS services, including contracts with NHS and private providers, in two parts of the new infrastructure – CCGs and NHS Local Area Teams.
- Under the new structure the resources spent on the work of commissioning and managing contracts, including managing contracts with NHS providers, are substantial. The 211 CCGs employ some 12,500 people, 20 and receive from central government around £25 per person whose healthcare they are responsible for to cover their running costs – a total of £1.3bn. For the 27 NHS Local Area Teams (which contract for NHS dentistry, pharmacy, ophthalmology and GP services) the available data suggest that there are around 3,440 employees, with a budget of £230 million.
- The remainder of this report focuses on the contracts that CCGs enter into with private providers. These follow a standard form drawn up by NHS England, but responsibility for the detailed provisions of each contract, and for ensuring that the terms of the contract are met, rests with CCGs.
- These contracts can be very complex. As Monitor notes: ‘health care commissioners often have to secure a huge number of different services from a single provider, meaning that negotiations between commissioners and providers can cover hundreds, sometimes thousands, of service lines’.According to the 181 CCGs which answered our survey, the average number of contracts held by each CCG with private sector providers was 90.
- These contracts are also of a qualitatively different nature from the nonenforceable contracts which existed in the NHS previously, and they lay heavier responsibilities on commissioners. They are negotiated privately between the parties and disputes can be litigated in the courts. The costs of negotiation and litigation may deter commissioners with limited budgets from undertaking effective enforcement of contracts.
- Such contracts are also confidential and not subject to the transparency requirements of the Freedom of Information Act. Commissioners’ rights to enter premises, inspect documents, interview patients, etc, are governed by the provisions of the contract itself. How far a contract confers such rights will affect the capacity of the commissioners to enforce it, and the absence of transparency makes third parties unable to tell whether a contract is in the public interest or whether it is performing well.
- Moreover, although individual CCGs are legally responsible for the contracts they make with NHS and non-NHS providers, their ability to hold providers directly to account is complicated by two factors.
- First, most CCGs contract out their contract management function to Clinical Support Units (CSUs). These bodies, of which in December 2014 there were 10, employ in total around 8,500 staff to undertake most of the contract management function for CCGs, and do so for up to 20 or more CCGs at a time.
- The exact legal and constitutional status of CSUs is unclear, which is a matter for concern given that they now play a central role in overseeing how large sums of public money are spent. They are in practice embryonic companies, initially consisting largely of staff who were previously employed by PCTs. At present they are ‘hosted’ by NHS England, but from April 2016 they are due to become fully private entities. CCGs currently pay them a total of around £700m a year for their services, or just over half the amount that CCGs receive from central government for their running costs. From February 2015 onwards CCGs which choose to outsource their commissioning work are required to put contracts for it out to tender when their current contracts expire. (See NHS England: Commissioning Support Lead Provider Framework Factsheet). NHS England has ruled two CSUs, which currently provide contract support for 47 CCGs, ineligible to compete to provide ‘end to end’ (i.e. comprehensive) services in future. They are expected to cease operation, while two other CSUs have announced plans to merge with a third in April 2015, leaving six remaining CSUs and three other private companies, to compete for all future end-to-end commissioning support contracts. One of the new companies is a consortium and another plans to use a ‘supply chain’ of additional companies to do some of work. In such cases the outsourcing of NHS clinical services will itself involve several levels of outsourcing. (See David Williams, ‘Jobs at risk as NHS England rejects two CSU bids’, HSJ 28 January 2015 and ‘Revealed: winners and losers of CCG support framework’, HSJ 5 February 2015).
- A second complication is that most CCGs collaborate with others in contracting for the provision of services for their respective populations. Typically, a single CCG will be the ‘lead’ commissioner with other CCGs joining in the contract as associate commissioners. The lead commissioner takes the lead in dealing with contractual performance issues on behalf of the associate commissioners.
- Both of these reasons may help to explain why 12 CCGs out of the 181 which responded to our survey were unable to tell us how many contracts they held with non-NHS providers.
- Health care is a complex good, meaning that it is very difficult to specify exactly what service is needed within a contract, making contracts for health care particularly difficult to monitor and enforce. Healthcare contracts also suffer from information asymmetry, whereby the commissioning body – in this case the CCG – will always know less about how well the contractor is performing than the contractor does. This makes it possible for contractors to ‘cheat’ or shirk on their contractual obligations and to provide false information about their performance.
- The incentive is intensified if the firm’s finances are under pressure, and in recent years some private providers of clinical services to the NHS have struggled to generate significant profits from contracts.
- These problems are not solely encountered by CCGs. In February 2014 the Public Accounts Committee (PAC) found that central government departments, with a total of £40bn in contracts with private sector providers, suffered acutely from asymmetry of information, and a severe imbalance of power and skills: The PAC found that there was ‘a longstanding problem of insufficient investment in staff with contract management skills.’
- The government’s Chief Procurement Officer told the Committee that ‘There has been an asymmetry between the suppliers and the officials. The suppliers sell deals, run deals and are earning big salaries. They have done it multiple times. Sometimes, they are up against officials who have none of those characteristics…’ The Committee concluded that ‘Government is clearly failing to manage performance across the board, and to achieve the best for citizens out of the contracts into which they have entered’.
- This raises the question whether 211 CCGs and ten CSUs, which are managing contracts with private providers worth £9.3bn, have the resources to do even as well as major government departments. In 2013 the economic regulator of the health service in England, Monitor, undertook a study of the effectiveness of local contracting within the NHS, interviewing CCGs and CSUs. The researchers found that the efficacy of local contracting was undermined by four factors.
- First, information asymmetry was a serious problem. They found that ‘providers have far better data than commissioners about the work they do and the costs of doing it, which they may be unwilling to share. Even where providers do share information, commissioners are not always able to have confidence in it because the quality of the information is sometimes poor’.
- Second, commissioners were ‘often at a disadvantage to providers in terms of both the scale of available resources (i.e. staff and time) and the skills and capabilities of those [in the] contracting teams. Both sides acknowledged that this can give providers the upper hand in contract negotiations’. Commissioners’ lack of contracting expertise increased the already high transaction costs of managing local contracts.
- Third, the threat of contract enforcement was not always credible. The report found that ‘Commissioners are sometimes reluctant to enforce contracts, particularly by imposing financial penalties, for fear of exacerbating providers’ existing problems’. Serco’s out-of-hours contract for Cornwall (Box 2) is an example of this.
Serco’s out-of-hours contract for Cornwall
From 2006 Serco had a contract to provide out-of-hours GP care services for the 500,000 residents of Cornwall. In June 2013 the Public Accounts Committee (PAC) reported that: ‘In early 2012 whistleblowers raised concerns that the out-of-hours service in Cornwall was short staffed and that the contractor, Serco, had lied about its performance by altering data… Evidence has confirmed that [this] was substantially true… Serco staff altered data on 252 occasions, resulting in Serco overstating the performance it reported to the primary care trust… Serco conceded that the contract manager had been paid a bonus which was linked to performance…’
At one point a single doctor had been on duty for the entire county. The Committee found that ‘The primary care trust did not scrutinise Serco’s performance effectively. When these issues came to light, it did not penalise Serco, withhold payment or terminate the contract.’
The former chair of the local Strategic Health Authority explained that ‘it has been our culture in the NHS not to levy fines and penalties, because… it often causes more problems by taking money away from places that are struggling.’ Commenting on this the Comptroller and Auditor General said that ‘dealing with a very large, powerful organisation that is all over the public sector is a bit different… when dealing with such an organisation, you probably need to be pretty robust in the way you defend your interests. You need to ensure that if you are entitled to anything or you have a point of leverage, you use it to the full.’
- Fourth, effective contract enforcement was also undermined by commissioners being dependent on providers: the report found that ‘lack of perceived or actual competition, reducing [the] provider’s appetite to perform to highest standards’, plus the knowledge on both sides ‘that the commissioner is reliant or critically reliant on the provider’, limited how effectively commissioners could enforce contracts.
- Many of these problems in monitoring and enforcing contracts with the private sector have manifested themselves in recent cases where failures in contract monitoring have led to patients being harmed, or put at risk of harm, or misleading information being provided to commissioners. It is significant that these cases have come to light as a result of a tragedy (Box 3), or whistleblowing, undercover reporting, or CQC inspections (Box 4), and not as a result of contract monitoring.
Box 3: Contracting for Out of Hours Care:
Take Care Now In 2008 a company called Take Care Now (TCN) had contracts to provide out-of-hours primary care for a total of 1.4 million patients in Suffolk, Cambridgeshire, Great Yarmouth and Waveney, South West Essex and Worcestershire. It had, however, great difficulty in recruiting and retaining staff and relied heavily on agency doctors from Europe. In February 2008 one of these gave a patient, David Gray, ten times the correct dose of dimorphine, which killed him.
A subsequent investigation by the Care Quality Commission found that TCN was persistently understaffed; that previous ‘near misses’ and Serious Untoward Incidents had not been properly recorded or learned from; that there had been official warnings about the use of dimorphine by agency doctors from European countries where this drug was not used; and that in general the company had shown an inadequate appreciation of its responsibilities for patient safety.
The CQC report also found that monitoring of the company’s contracts by the commissioning PCTs had been extremely weak:
‘The staff in the PCTs with responsibility for routine monitoring of the contracts for out-of-hours did not understand TCN’s reports on performance. They could not adequately explain the data or the basic activity figures… Before the start of this investigation, none of the PCTs robustly monitored staffing levels, skill mix or whether the shifts were filled, and most did not monitor them at all. The PCTs did not have a clear picture of problems in out-of-hours services. They were not generally aware of serious incidents. None of the PCTs had robust established arrangements to share information on poorly performing clinicians.’
- These cases where private providers have failed to perform make it clear that the information asymmetry can only be truly overcome through site visits to providers. We therefore asked how many times CCGs visited the sites where NHS-funded services were being provided by non-NHS providers as part of the CCGs’ contract monitoring work. Whilst many CCGs told us that their contract monitoring involved meeting regularly with private providers of NHS services, we thought it would be useful to identify how often actual site visits took place. Interestingly, a large number of CCGs (109 out of the 181 which responded) were unable to answer because they didn’t record this information. Of those that did record how many site visits had been made between April 2013 and October 2014, 22 reported that they had not made any, while 39 had undertaken fewer than 10.
Box 4: The Spire Wellesley
In June 2013 an NHS patient at the private Spire Wellesley hospital in Southend received a ‘wrong site’ joint replacement implant. Wrong site surgery is a ‘never event’ – a ‘serious, largely preventable patient safety incident that should not occur if the available preventative measures have been implemented by healthcare providers’ – but it was only a year later, after two further wrong site implants had occurred, that a CQC inspector learned about the NHS patient’s case from hospital staff.
The CQC inspector noted that approximately 37% of the Spire Wellesley’s patients were NHS patients, but that there were ‘marked differences between the NHS process and Spire Hospital’s adverse event /near miss reporting policy. The Spire policy… lacked detail of how a serious or never event should be reviewed to ensure practice changes and lessons are learnt to prevent a reoccurrence… only one member of staff had received appropriate training in investigation management… Whilst the clinical effectiveness committee discussed serious incidents this was rarely shared formally with junior staff in the clinical areas or the Resident Medical Officer.’
Contract monitoring by the CCG had failed to ensure the safety of NHS patients treated at the hospital. In August 2014 the chair of the CCG’s Quality, Finance and Performance Committee asked why no contract report was available, ‘as despite issues with quality and safety at Spire Wellesley that have been raised by the CCG and CQC, we are still sending more patients there…’
- The former Chair of the Strategic Health Authority in the Serco case told the Public Accounts Committee that ‘it has been our culture in the NHS not to levy fines and penalties, because… it often causes more problems by taking money away from places that are struggling’ (see Box 2 above). This suggests a disincentive to use financial sanctions to enforce a contract even when a provider was seriously failing.
- We therefore also asked how many contracts with non-NHS providers had been terminated because of poor performance and how many sanctions had been applied. Of the 15,166 such contracts that were held by CCGs only seven had been terminated. In terms of financial sanctions imposed under contracts with non-NHS providers, 149 CCGs said that they had imposed none; sixteen had imposed financial sanctions totalling £3.8 million, although in relation to £1.9m of this no monies were permanently withheld, so it is unclear whether it amounted to a sanction. A hundred and thirty three CCGs had not issued any contract queries since 2013 in relation to the contracts that they held with nonNHS providers.
- Finally it should be noted that two CCGs said they could not provide us with information on the number of staff employed in contract monitoring, or the number of site visits undertaken, because it was commercially sensitive information belonging to the CSUs they were employing. One stated that ‘The CSU’s ability to apply for tender of future contracts would undoubtedly be harmed if the details you have asked for are disclosed and it would be significant: in our opinion this prejudicial effect outweighs the public’s right to know how public funds are spent’.
- If such information is deemed to be commercially sensitive after April 2016, when it is intended that all commissioning support will be provided by private companies (including CSUs, which will then also become private companies), it will not be possible to know how CCGs which use CSUs are exercising their responsibilities under the Health and Social Care Act 2012.
Conclusion and recommendations
- The Health and Social Care Act 2012 marked the final step in the creation of an external market for NHS care, a market underpinned by a myriad of contracts, increasingly being held between the NHS and private providers of healthcare.
- All the contracts which underpin the NHS market, including contracts with NHS providers, require administration of one form or another, and there are now some 25,000 staff employed by the NHS in this endeavour. These staff are spread between Local Area Teams (3,400), which manage primary care, dental, ophthalmic and pharmacy contracts, and CCGs (12,500) and CSUs (8,500), which manage secondary care and community health contracts, at an estimated total annual cost of £1.5bn.
- However, there is a significant lack of information about how this resource is used in practice, and how effective it is. As both Monitor and the Public Accounts Committee have found, acquiring the expertise and the resources for contracting effectively with private providers is a serious problem. The data provided to us by CCGs provide evidence of the challenges that CCGs face, but also raise significant questions about the transparency of the contracting arrangements, and about who is exercising the powers granted to CCGs under the Health and Social Care Act.
- If the outsourcing of NHS clinical services to the private sector is to continue, and if patients and the public are to be confident that standards are being met and that value for money is achieved, a number of measures need to be taken to address the issues raised in this report.
- NHS England should commission an independent audit of CCGs’ capacity to monitor and manage contracts with non-NHS providers before any further major contracts are arranged.
- NHS England should re-consider its plans to privatise the contract monitoring of NHS contracts. CCGs are the statutory bodies responsible for enforcing contracts between the NHS and the private sector, not CSUs, which remain unaccountable if anything goes wrong. This problem will be exacerbated if CSUs become private companies, as is intended, from April 2016. With nearly £10bn worth of contracts with the private sector already in place, it is vital that statutory bodies are genuinely responsible and accountable for ensuring that private providers deliver according to the terms of their contracts.
- To increase transparency CCGs should be required to publish regular performance data on the number and value of contracts they hold, how they know whether contracts are performing well, the number and type of staff they employ to monitor and enforce contracts, and the amount of any overpayments they may have made to providers due to fraud or error.
This report was produced by the CHPI research team with the assistance of Laura Stoll and Mubeen Bhutta and is reproduced with their kind permission.
