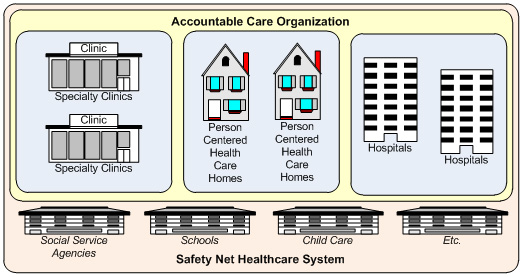
It has become de rigueur on the left to regard the US healthcare system as the very incarnation of evil and therefore a country from which nothing of value can be learned for improving our NHS. This might be about to change. There is now growing interest in the notion of the ‘Accountable Care Organisation’ (ACO) – or as it is tending to be termed over here, the Accountable Integrated Care System.
The Accountable Care Organisation concept is gathering pace in the US following the 2010 Patient Protection and Affordable Care Act, which included a pilot programme to explore ACO structures and processes. Under the new law, an ACO would agree to manage all of the healthcare needs of a minimum of 5,000 Medicare beneficiaries for at least three years. The ACO can gain extra money through sharing savings (with Medicare) resulting from collaborative efforts to provide care cost-effectively. Stringent governance conditions must be met, along with transparency and quality performance – Medicare ACOs will report on 33 different quality metrics.
In his recent ‘Green Paper’ speech on future Labour Party health policy, Andy Burnham spoke of the need for “one service co-ordinating all of one person’s needs“, with the district general hospital “evolving over time into an integrated care provider from home to hospital“. Indeed, he went on to say:
“If we look to the US the best providers are working on that highly integrated basis, co-ordinating physical, mental and social care from home to hospital. We have got to take the best of that approach and universalise it here.”
This certainly seems to resemble the Accountable Care Organisation model whereby a ‘prime contractor’ takes on the budget and responsibility for selected groups of patients, and commissioners offer financial rewards for reaching agreed outcomes-based goals. It is an approach that seeks to address several current problems that bedevil healthcare provision in both countries:
- payment by activity models have simply fuelled hospital-based activity
- commissioners have focused narrowly on silo-based micro-commissioning
- service delivery has been fragmented and uncoordinated
- ‘pure’ contractualisation is insufficient to bring about provider change
- nobody is accountable for integration
The Accountable Care Organisation model would not abolish the purchaser-provider split, and therefore falls short for those wishing to settle for nothing less – indeed, if anything, the model would require commissioning expertise of an order and scale hitherto unattained. The ACO approach tends to assume that the ‘system goal’ is to reduce unnecessary and inappropriate dependence on expensive hospital facilities, and to shift resources into care closer to home. Robust measures of process, outcome and patient experience to reflect this goal would therefore need to be developed and monitored by the commissioners.
As Burnham suggests, acute hospitals will be in pole position to assume the role of ‘main contractor’, especially where they already contain community health services. The task of the main contractor would be to ensure delivery of an agreed pathway of care by drawing on a wide range of collaborating organisations and professions within and external to the traditional bricks and mortar focus. Depending on the scale of ambition this could be expected to include other statutory partners across health and local government, the third sector and also private providers if appropriate. On the commissioning side there is no reason in principle why stronger health and wellbeing boards could not act as the single integrated commissioning organisation for this model, hence avoiding structural upheaval.
This would need very careful planning. Amongst the key considerations will be:
- patient choice: government policy is to privilege patient choice above other considerations, and it is not clear how patients can have a choice of ACO
- upfront investment: the main contractor will need a single information system that can engage with all of the systems of sub-contracted agencies
- provider capture: there is always the danger that where the commissioning is weak, hospitals will simply ramp up their in-patient activity
- public and patient involvement: the bottom-line for public sector organisations is defensible decision-making, and both commissioners and contractors would need genuine buy-in from the public
The Accountable Care Organisation model is capable of covering very different degrees of ambition on the part of commissioners and providers, and the trick could be to select a ‘frame’ that is commensurate with local history and capacity. Whilst some localities might restrict themselves initially to issues such as diabetes and visual health, others could go for the bigger beasts, notably frail elderly people with complex long-term conditions. However the assumption must be that modest ambitions are widened on a frequent basis, otherwise the model would simply be a replicate of silo-based micro-commissioning of the sort seen with GP fundholding.
This is all uncharted territory, even in the USA, but it is obviously attracting political interest in England. As well as the interest being shown by Andy Burnham, the model seems to be in the thinking of the Lib Dem Health Minister, Norman Lamb. There is no doubt Lamb would like to see a big push on integrated care, and it was reported in November last year that he was planning to support a series of large-scale integrated care ‘experiments’ that could allow local health economies to devise their own payment systems and move away from the straitjacket of ‘payment by results’. Moreover it was mooted that this could also involve an assurance that Monitor would not act to break up collaboration on anti-competitive grounds.
This sort of talk will not attract those who simply wish to see an end to the purchaser-provider split and the return of an entirely ‘in-house’ system, but it could serve as a bulwark against the more aggressive forms of marketisation favoured by the Coalition. The newly published procurement regulations, for example, lay down that:
- all providers must be treated equally, ‘particularly on the basis of ownership’
- commissioners ‘must not engage in anti-competitive behaviour’ and should ‘not include any restrictions on competition that are not necessary’
- a contract can only be awarded without competition ‘for reasons of extreme urgency’
The procurement regulations reflect the complex policy world within which local partners now have to work. To blindly go along with them will inevitably lead to a fragmented and increasingly privatised NHS. To keep them at bay requires a plan. Could the Accountable Care Organisation be just such a plan?
Professor Bob Hudson,
School of Applied Social Sciences, University of Durham