Prescription charges have been a symbolic issue since Aneurin Bevan resigned from the Labour Government on 23 April 1951. This is often claimed to be on the issue of prescription charges, but his resignation speech makes it clear that prescription charging was only a small part of the argument, and in fact the Labour Government did not introduce any charges. He had earlier gone along with the introduction of a power to make a charge in 1949 in the NHS Amendment Act.
Charges were actually brought into force 1952 by the Conservative government at a rate of 1 shilling per prescription. There were exemptions for people in receipt of National Assistance, War Disability Pension, children under 16 or at school, and venereal disease patients.
In 1956 rules were changed so that the charge applied to each item prescribed. In 1961 it was doubled to 2 shillings, and charges were abolished by the Labour Government on 1/2/1965, only to be reintroduced on 10/6/1968 at a higher rate of 2 shillings and six pence but with a wider range of exemptions. In April 1971 the prescription charge was increased from 12.5p to 20p. In 1974 the exemption for children was raised to 16 and for women reduced to 60. The Conservative government then consistently increased the charge above the rate of inflation. In England 2012 the prescription charge is now £7.65.
In 1949 there wasn’t much effective medication. Prescription charges were seen mainly as a way of reducing the quantity of medicine pouring down the nation’s throat. But now there is a lot of very effective medication which, when taken, reduces the need for more expensive hospital treatment. So it doesn’t make much sense to discourage poor people from taking their medicine. Gordon Brown announced that cancer patients will not pay charges from April 2009. The plan was that free prescriptions would then be introduced for people with long term conditions – a plan that was derailed by the financial crash. But the more people are exempt the greater the cost of administration compared with the revenue.
The Prescription Charges Review for those with Long Term Conditions included a web survey – the closing date was 27 February 2009.
The central question asked was:
- Which of the following factors should govern whether a person with a long term condition should be entitled to receive free prescriptions?
- How severe the condition is and how seriously it affects the person’s quality of life?
- How long they have suffered from the condition?
- They suffer from the symptoms all or most of the time (rather than people with symptoms that come and go)?
- The amount of treatment required to keep the condition under control?
- The potential to improve the person’s health?
Which other factors do you think are important?
We think economic factors are more important. It is hard to see how the factors listed can be turned into a policy which is fair and makes sense. In 2009 anyone whose weekly income was more than £3.65 above the Income Support poverty line had to pay the full cost. For single people under 25 – £51.60; 25 or over – £64.15. That means that many people on Incapacity Benefit long-term basic rate – £84.50 – had to pay in full. If you can’t find £7.10 it doesn’t matter which category you come in.
Experience from CABx shows that many people on Incapacity Benefit have wrongly assumed that they were entitled to free prescriptions. This can result in patients facing accusations of fraud, penalty charges and even threatened prosecution. This is despite the fact that it seems probable that the vast majority are cases of error rather than deliberate fraud, and where the underlying problem is one of poverty. Moreover there is no formal means of appeal against such a decision.
The penalty charge is five times the charge that the client should have paid, up to a maximum of £100. The client will also be asked to pay the original charge itself. If the client does not prove her/his entitlement to help with health costs, and s/he does not pay the amount stated in the penalty charge notice, the NHS may take court action to recover the debt. The penalty charge is increased by 50 per cent of the penalty charge if s/he does not pay within 28 days of the date the penalty charge notice is sent.
Wales abolished prescription charging on 1 April 2007. Free Prescriptions: A Welsh Solution To Welsh Health Problems Wales leads the way as prescription charges fall
Northern Ireland’s Health Minister announced on 29 September 2008 that they will phase out prescription charges by 2010 subject to the agreement of the Executive. Prescription charges will reduce to £3 in 1 January 2009 (from the then current £6.85). Free prescriptions gets green light
The Scottish Government announced on 5 December 2007 how they will phase out prescription charges by 2011.Scotland abolishes prescription charges
The Netherlands abolished prescription charges in 2008. All Dutch residents aged 18 and over must pay the first E150 per year of their non-hospital health care costs, but this does not include GP care, preventive care, mother and child care, prescription drugs or (for those under 22 years) dental care.
Report of the Prescription charges review: implementing exemption from prescription charges for people with long term conditions. Pleased to see that Prof Gilmour accepted most of the arguments we put.
-
-
- Abolish Prescription Charges – Swindon TUC’s campaign
- CAB evidence on prescription charges 2009:
-
-
- Free Prescription Charges in England 2009 seminar
- Health committee report on NHS Charges July 2006 Government response October 2006
- NHS Costs – official guidance
- MORI poll 2008commissioned by Citizen’s Advice
- NHS Low Income Scheme
- Prescription charges – planned new exemptions Jan 2009
- A prescription for the economy – better health in the long term/ 2012
- Prescriptions policy is ‘dog’s dinner’ (Social Market Foundation 2004)
- Royal Pharmaceutical Society of Great Britain presentation 2009:
- Scottish Campaign to Remove All Prescription Charges
- Scrapping prescription charges could drive up drugs bills 2009
- Unhealthy charges: CAB evidence on the impact of health charges
- What impact do prescription drug charges have on efficiency and equity? Evidence from high-income countries2008
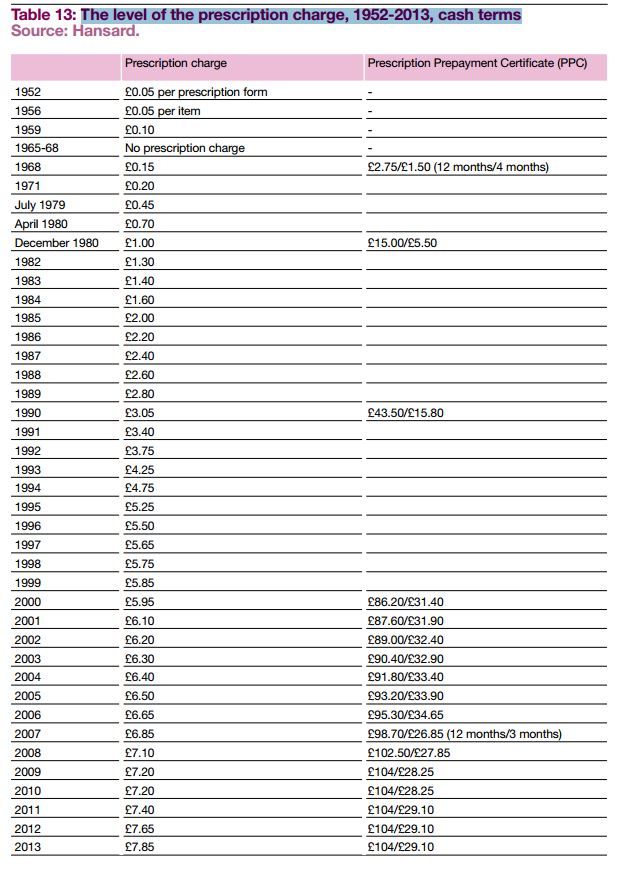
This helpful table is taken from The cost of our health: the role of charging in healthcare, Reform 2013